📖 Read more: Greenland Sharks: Living 500 Years Defying Aging
🩸 Blood Vessels: Far More Complex Than We Thought
Blood vessels resemble the highways of a metropolis — full of curves, branches, merges, and traffic bottlenecks. Every curve, every narrowing dramatically changes how blood flows and the forces exerted on vessel walls. It is precisely at these points — where geometry becomes complex — that most vascular diseases develop: atherosclerosis, thrombosis, aneurysms.
Yet for years, laboratory blood vessel models were simplistic — straight channels without branches or curves. Useful, but extremely limited: they could not reproduce the conditions under which vascular diseases actually develop. This means that drugs tested on these simplified models often failed when tried on patients — at enormous cost in time, money, and human lives.
🔬 The Texas A&M Vessel-on-a-Chip
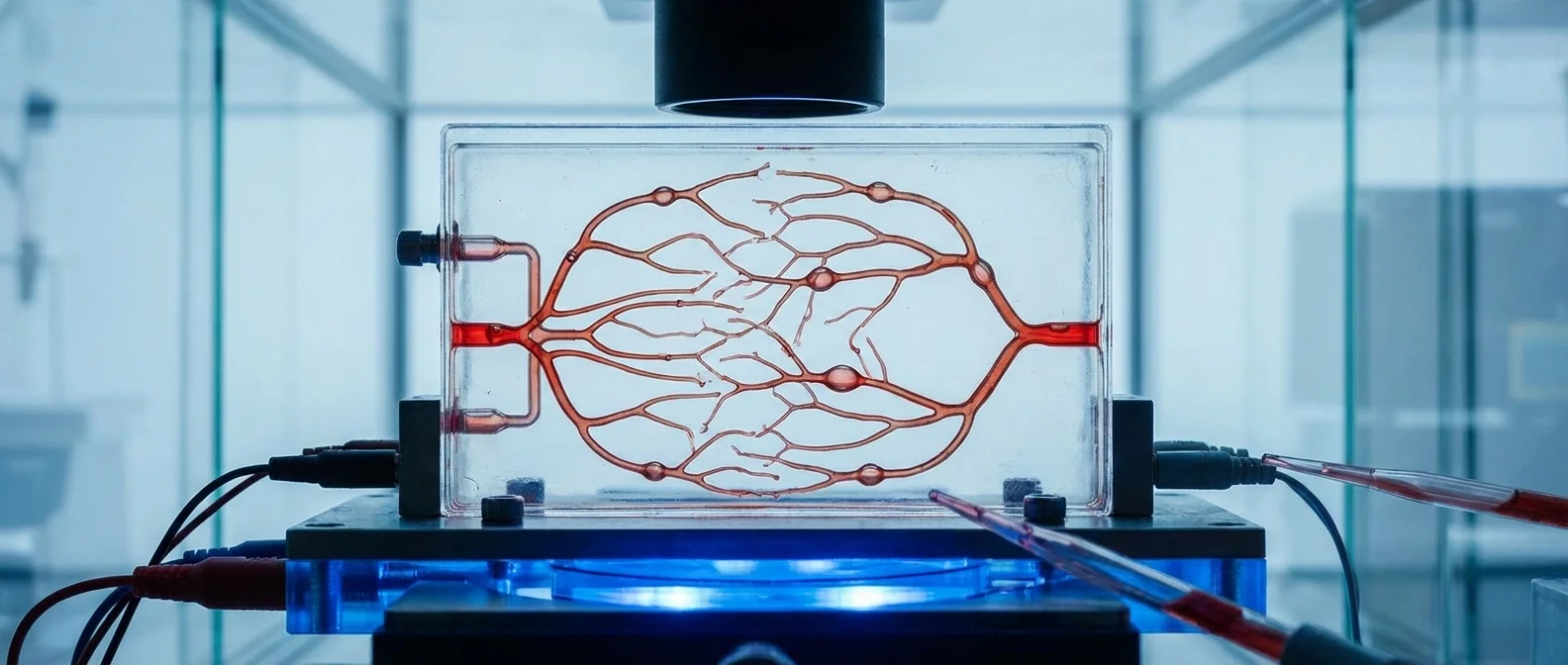
Researchers at the Department of Biomedical Engineering at Texas A&M University decided to change this landscape. Under the guidance of Professor Abhishek Jain, graduate student Jennifer Lee designed an advanced “vessel-chip” — a microfluidic device that reproduces the real architecture of human blood vessels on a microscopic scale.
Unlike previous straight-vessel models, the new chip includes branches, stenoses, and aneurysms — precisely the structures that make blood flow so complex in the human body. Lee explains: "There are branching vessels, aneurysms with abrupt widening, and stenoses that constrict the vessel. All these types of vessels significantly alter blood flow patterns and the inner surface of the vessel is affected by shear stress levels. That's what we wanted to model."
The research was published in the scientific journal Lab on a Chip and is set to grace the cover of the May 2025 issue — a recognition of the work's significance.
🧪 How the Vessel-Chip Works
The chip is a microfluidic device — a silicone plate smaller than a postage stamp, containing microscopic channels. Living human endothelial cells (those that line the inner walls of blood vessels) grow inside these channels, creating functional blood vessels. Nutrient fluid simulating blood flows through, exerting the same forces the cells would experience in the body. Researchers can change the geometry, flow rate, and add drugs, observing in real time how the vessels respond.
📖 Read more: Nanolaser on Chip Cuts Computer Energy 50%
🧬 The Fourth Dimension of Organ-on-a-Chip
What makes this particular innovation stand out is not just the complexity of its geometry, but the fact that the vessels are alive. These are not static models or 3D prints — the cells grow, respond to stimuli, become inflamed, and form clots exactly as they would inside the human body.
Dr. Jain describes this development as the “fourth dimension” of organ-on-a-chip technology: "We are no longer focusing only on cells and flow, but on the interaction of cells and flow within complex architectural structures. This is a new direction for the field." Future versions of the chip will incorporate multiple cell types — not just endothelial cells — to study how different tissues interact with each other and with blood flow.
"We can now learn about vascular diseases in ways that were never possible before. You can not only make the structures complex, but put real cellular and tissue material inside them and make them alive. These are the spots where vascular diseases tend to develop."
💊 Why This Is a Game-Changer for Drug Testing
Cardiovascular diseases remain the leading cause of death worldwide, killing approximately 17.9 million people every year according to the World Health Organization. Yet the development of new drugs for these diseases is extremely slow and expensive — mainly because existing laboratory models and animal experiments fail to predict how the human body will respond.
The vessel-chip addresses exactly this problem. Thanks to its realistic geometry and living cells, it can reveal how a drug affects blood flow in narrowed vessels, whether it causes inflammation at branching points, or whether it increases the risk of clotting near an aneurysm. Information that a simple straight-vessel model could never provide.
📖 Read more: Photons Mimic Brain Function: Quantum Neuromorphic Memory
🐾 Reducing Animal Experiments
One of the most significant advantages of vessel-on-a-chip technology is the potential for drastically reducing animal experiments. Every year, over 100 million animals are used in laboratory testing worldwide — and yet, the results often do not translate to the human body. Mice do not develop atherosclerosis like humans, their vessels have a different structure, and their metabolism differs significantly.
Vessel-chips, by contrast, use human cells in human-like architecture. They can even be personalized per patient — using cells from the patient themselves to create a model that reflects their own vascular biology. This opens the door to personalized medicine: testing drugs on a patient's “digital twin” before administering them to their actual body.
🌐 A Broader Innovation Ecosystem
The Texas A&M work does not exist in a vacuum. It is part of a rapidly growing field of “organ-on-a-chip” that includes lungs, kidneys, brains, and even entire “body-on-a-chip” systems — platforms that connect multiple micro-organs in a single circuit to simulate the entire human body. Meanwhile, researchers at Western University recently captured for the first time on a chip the process of intussusceptive angiogenesis — the way a blood vessel splits into two, a process critical in wound healing as well as in the growth of cancerous tumors.
The project's funding reflects its significance: it is supported by the National Institutes of Health (NIH), NASA, the U.S. Army, the FDA, the National Science Foundation (NSF), and BARDA (Biomedical Advanced Research and Development Authority). Such interdisciplinary support shows that this technology is not merely an academic experiment — it is a strategic priority for public health, defense, and space.
🔮 What This Means for the Future
Vessel-on-a-chip technology is still in its early stages, but the path it charts is clear. In the near future, pharmaceutical companies will be able to evaluate new compounds on complex, realistic vessel models before proceeding to clinical trials — reducing cost, time, and the number of animals used. In the long term, integrating multiple cell types, linking multiple chips, and using artificial intelligence for analysis will create virtual human bodies on which every drug can be tested before it even touches a real patient.
Jennifer Lee, who started as an undergraduate student with no knowledge of organ-on-a-chip technology, managed within a few years to publish research that changes the rules. Her story is a reminder that science always advances thanks to people who dare to look beyond straight-line models — both literally and figuratively.
📚 Sources
- 🔗 ScienceDaily — Scientists just made living blood vessels on a chip that act like real ones (Feb 2026)
- 🔗 Phys.org — Customizable chips mimic real-life blood vessel structures for disease research (May 2025)
- 🔗 Lab on a Chip — Vascular architecture-on-chip (Lee, Kumar, Mathur & Jain, 2025)
- 🔗 Phys.org — Microfluidic device captures blood vessel splitting in action (Aug 2025)
- 🔗 New Atlas — Body-on-Chip system mimics the behavior of 10 connected organs